Background
Relationship difficulties in healthcare settings have been reported as a factor leading to nurses leaving the workforce (Kashiwada, 2018). Seitovirta et al. (2018) suggested the creation of a cordial team environment where nurses feel comfortable sharing their opinions. They also recommended providing numerous opportunities for the team to reflect on nursing practice individually and as a team. Gregg et al. (2017) reported that novice nurses require “resilience to overcome periods of confusion” and the “acquisition of interpersonal skills to create a safe human environment for learning” in order to learn how to work as a nurse in a clinical setting. Effective communication and interaction enable nurses to develop caring, empathetic, and respectful relationships with patients and their families.
Healthcare relationships worldwide are characterized by hierarchy and power dynamics, which are particularly complex in Japan. Cultural values regarding hierarchy and power persist alongside differences in professional status, gender imbalance, seniority/generation gap, bullying, and humility/ modesty, all of which impact Japanese nurses’ assertive communication in their daily practice (Omura et al., 2018).
For healthcare professionals, clinical self-efficacy and competency are essential for providing quality healthcare and ensuring patient safety (Dellafiore et al., 2022; Shorey & Lopez, 2021). Dispositional humility is a character trait that enables one to control self-centered professional impulses and be attentive to the needs of other professionals. Limiting self-interest while focusing on the needs of others may be necessary and in the best interest of patients to maintain quality patient care while working as a team (Sasagawa & Amieux, 2019). Nurses also need to employ self-care strategies, such as emotion regulation and self-compassion, to reduce their vulnerability to caregiving fatigue and improve their well-being and resilience (Hofmeyer et al., 2020).
It becomes clear that interpersonal skills are essential in preserving well-being and preventing turnover for novice nurses. Existing instruments that measure interpersonal competency were developed with student nurses (Dearing & Steadman, 2009), a scale was designed to measure interpersonal communication competency in undergraduate and graduate nursing students (Klakovich & dela Cruz, 2006), and another one targeted Japanese psychiatric outpatients and university students (Matsudaira et al., 2008). None of the instruments found in the literature focus on novice nurses in a challenging adjustment phase of their professional careers; therefore, this study aimed to develop and psychometrically test the perception dimension of the Professional Interpersonal Competency Assessment Scale for Novice nurses (PICASN) in Japan. The scale is designed to clarify the interpersonal skills and competency required of novice nurses based on Japanese cultural characteristics.
Literature Review
In a complex healthcare system, effective teamwork is essential for patient safety by minimizing adverse events caused by miscommunication with other healthcare providers and misunderstanding of roles and responsibilities (Babiker et al., 2014). Thus, novice nurses require soft skills and competency. According to literature, soft skills are the personal attributes and social intelligence that enable someone to interact effectively and harmoniously with others. Soft skills for the healthcare field can be learned and developed over time through practice (Taylor, 2022). The areas covered include empathy, communication skills, teamwork, work ethic, stress management, positive attitude, flexibility, time management, professionalism, and self-development (Oduenyi, 2022). The concept of social competency involves an individual’s ability to interact effectively and appropriately with others. In Japan, people are expected to know without explicit communication what the other person wants to express or desires (Matsudaira et al., 2008). The difference between perceptual and behavioral aspects is critical. An imbalance in an individual’s perceptual abilities can lead to difficulties at the social level, that is, at the interpersonal level (Bolis & Schilbach, 2018).
In 1992, Roach identified the five Cs of caring (compassion, competency, commitment, confidence, and conscience) and added a sixth C (comportment) in a second edition in 2002 (Baillie, 2015; Roach, 2002). Nurses are expected to demonstrate the six Cs of nursing in “everything we do” (Duffy, 2015). Patient-centered care is defined as “care that respects and responds to individual patient preferences, needs, and values, and ensures that patient’s values guide all clinical decisions” (Newell & Jordan, 2015). Institute of Medicine et al. (2003) propose a set of core competencies for health professionals: providing patient-centered care-identifying, respecting, and responding to patients’ differences, values, preferences, and expressed needs; alleviating pain and suffering; coordinating continuity of care; listening to, clearly informing, communicating with, and educating patients; sharing in decision making and management; and continually advocating for disease prevention, wellness, and promotion of healthy lifestyles, including a focus on population health (Institute of Medicine et al., 2003).
It is noteworthy that establishing a therapeutic patient-nurse relationship anchors on a positive bedside manner, including effective communication, empathy, respect, and professionalism, while practicing attending skills and offering honest, encouraging, and integrity-driven care (Davidhizar & Shearer, 1998). Each person grows in their ability to express caring throughout their life. Each nurse grows in their competency to express themselves as a caring person (Boykin & Schoenhofer, 2001). The recent version of the Technological Competency as Caring in Nursing theory (Locsin & Purnell, 2015) explains that in the process of knowing, persons are appreciated as participants rather than objects of care.
Methods
The development of the instrument was divided into four steps: 1) concept identification, 2) item construction, 3) validity measure, and 4) reliability measure (Davis, 1996).
Step 1. Concept Identification
To comprehend the concept under study, the researchers conducted a previous study exploring the necessary professional interpersonal skills required by novice nurses (Sato & Yasuhara, 2023). Two Professional Interpersonal Competency for Novice Nurses were identified: 1) Soft skills (empathy, communication skills, teamwork, work ethic, stress management, positive attitude, flexibility, time management, professionalism, and self-development), and 2) Interpersonal competency (person-centered care, compassion, competency, commitment, confidence, and conscience, behavior, and knowing the patient).
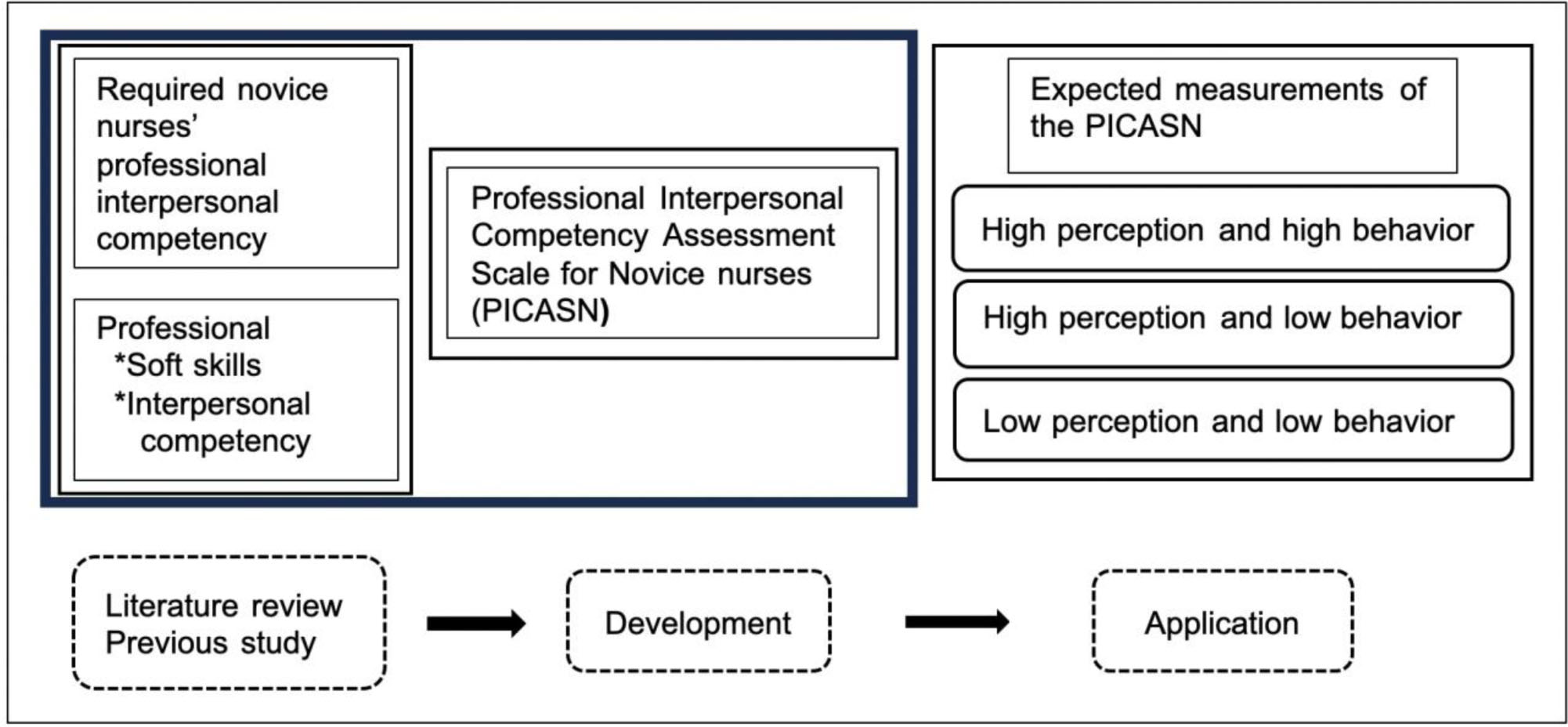
Semi-structured interviews were also conducted among nurses with 3-5 years of experience in two acute care hospitals. Nurses in their 3rd to 5th year of practice have both the experience of being a novice and a senior nurse. Eleven nurses (one male and ten females) were invited to participate in this research, and consent was obtained from all of them. The mean age of the nurses was 25.0 years. The interviews ranged from 22 to 39 minutes per person and were conducted using an interview guide. Participants were asked a) about their own experiences as new nurses, including difficulties in communication, and b) what skills are necessary for new nurses to establish good relationships during training. Additionally, a literature review was conducted using published resources to search for possible items in the scale. Overall, the in-depth interviews and literature search generated a total of 42 items. The process of developing and using the PICASN is illustrated in Figure 1.
Step 2. Item Construction
For this step, a panel of experts was assembled, comprising five clinical nurses with 3-10 years of experience, one professor, and four faculty members from nursing universities in Japan. They were tasked with determining the item format and scoring schema of the instrument. The consensus was that a 5-point Likert-type scale should be used to describe scaling responses. Participants responded by selecting one of five options: 1) Not Important, 2) Slightly Important, 3) Moderately Important, 4) Important, and 5) Very Important. Among the ten experts, this step had an 80% agreement rate.
Step 3. Validity Measure
The validity of the instrument was assessed through face, content, and construct validity. For face and content validity, the panel of experts (same experts as Step 2) reviewed the 42 draft items of PICASN. Linguistic item modifications were made to fit the cultural context. In terms of content validity, each item is rated as 1 (not relevant) or 2 (highly relevant). The item-content validity index (I-CVI) and the scale-content validity index (S-CVI) were then calculated, and items with a content validity index of 0.8 or higher were used and considered acceptable (Polit & Beck, 2010). Davis (1992) also recommends a CVI value higher than 0.70.
For construct validity, exploratory factor analysis (EFA) using maximum likelihood estimation with Promax rotation was used to assess the factor structure of the perceptual dimension of the PICASN. The CVI and the item-rest (I-R) correlation were examined in parallel with the EFA to determine the number of factors.
The participants in this study included novice nurses with 1-2 years of experience from 19 Japan Council for Quality Health Care accredited hospitals in the Chugoku and Shikoku regions of Japan.
The survey was conducted from February to April 2023 using Survey Monkey for data collection, especially for psychometric testing with EFA. Letters of invitation to participate were sent to the directors of nursing, who agreed to distribute the document containing the URL to facilitate survey participants’ access to the survey instrument. The invitation letter included the study’s purpose, the research collaboration process, ethical considerations, and a URL and QR code to access the survey website.
The questionnaire collected data on the respondents’ age, gender, work unit/department, and hospital function. Three questions regarding perceptions of the work environment were rated on a 4-point Likert scale: 1) strongly disagree, 2) disagree, 3) agree, and 4) strongly agree. The generated PICASN (42 items) were rated on a 5-point Likert scale: 1) strongly disagree, 2) disagree, 3) neither agree nor disagree, 4) agree, and 5) strongly agree.
The collected data were analyzed using Jamovi (version 2.3.21) (https://www.jamovi.org/) to assess the psychometric properties of the instrument with EFA using maximum likelihood with Promax rotation. Sampling adequacy was assessed using the Kaiser-Meyer-Olkin (KMO) test, with values >0.6 considered good (Li & Lopez, 2007). Bartlett’s sphericity test was used to examine the null hypothesis that the variables are not correlated in the population (p <0.05) (Tabachnick & Fidell, 2007).
In this study, Bartlett’s test of sphericity was highly significant (p <0.001), indicating that the dataset was suitable for the reduction technique. The Kaiser-Meyer-Olkin (KMO) measure of sampling adequacy was 0.93, demonstrating that factor analysis was appropriate for these data.
As a rule of thumb to assess the significance of factor loadings, factor loadings of 0.3 to 0.4 are minimally accepted (Hair et al., 2010). Factor loadings below 0.30 are typically ignored; a better cut-point would be 0.40 (Brown, 2009). The number of factors with eigenvalues greater than 1.0 were considered, and factor loading coefficients of 0.40 and greater were selected as the criterion for retention. The total score and the mean factor score (MFS) of the PICASN were calculated. The significance level was set at p <0.05.
Step 4. Reliability Measure
The reliability of the instrument was assessed using Cronbach’s alpha coefficient. I-R correlation values were calculated when items with a value of 0.6 or higher were employed. The ideal Cronbach’s alpha coefficient value is at least 0.70 (Polit & Beck, 2010).
Ethical Considerations
The ethical approval for this international study was obtained from the Ethics Committee of Tokushima University Hospital, Japan, (approval number 3610-3). The consent form was provided through the link before the survey questions and was only accessible if participants agreed to participate.
Results
Demographic Characteristics of the Participants
Survey questionnaires were distributed to 797 novice nurses. Complete data from 203 participants were included in the analysis, resulting in a final response rate of 25.5%. Table 1 displays the demographic characteristics of the study participants. There were 20 (9.9%) males and 183 (90.1%) females. The majority were 23-24 years (53.7%), with a mean age of 24.1 ± 4.59 years. Eighty-four (41.4%) participants worked at public hospitals, and 75 (36.9%) were at private hospitals. The areas of assignment included mostly the Department of Surgery with 79 (38.9%) and the Department of Internal Medicine with 60 (29.6%). Regarding the questions related to the work environment and turnover, most had been scolded by a senior nurse. Moreover, the majority of the participants felt that the atmosphere in their department was good and expressed a desire to continue working in their current hospitals.
| Characteristics | n | % | |
|---|---|---|---|
| Gender | Male | 20 | 9.9 |
| Female | 183 | 90.1 | |
| Age (Mean ± SD) 24.1 ± 4.59 years | 21~22 years old | 64 | 31.5 |
| 23~24 years old | 109 | 53.7 | |
| 25~29 years old | 17 | 8.4 | |
| Over 30 years old | 13 | 6.4 | |
| Hospital type | National University Corporation | 28 | 13.8 |
| Independent Administrative Law Firm National Hospital Organization | 16 | 7.9 | |
| Public hospitals (city, town, village) | 84 | 41.4 | |
| Private hospital | 75 | 36.9 | |
| Department | Department of Internal Medicine | 60 | 29.6 |
| Department of Surgery | 79 | 38.9 | |
| Intensive care (Emergency Room, Intensive Care Unit, Operating Room) | 40 | 19.7 | |
| Pediatrics, Obstetrics and Gynecology | 21 | 10.3 | |
| Psychiatry | 3 | 1.5 | |
| Questions related to work environment and turnover | |||
| 1. Have you ever been scolded by a senior nurse? | Strongly disagree | 18 | 8.9 |
| Disagree | 50 | 24.6 | |
| Agree | 78 | 38.4 | |
| Strongly agree | 57 | 28.1 | |
| 2. Do you feel that the atmosphere in your department is good? | Strongly disagree | 7 | 3.4 |
| Disagree | 18 | 8.9 | |
| Agree | 105 | 51.7 | |
| Strongly agree | 73 | 36.0 | |
| 3. Would you like to continue working at your current hospital? | |||
| Strongly disagree | 24 | 11.8 | |
| Disagree | 57 | 28.1 | |
| Agree | 93 | 45.8 | |
| Strongly agree | 29 | 14.3 | |
Validity Measure Results
It is noted that the examination of EFA, CVI, and item-rest (I-R) correlation was conducted concurrently with the EFA to determine the number of factors. The initial I-CVI and S-CVI of the ten nursing experts were 0.84 and 0.69, respectively. The mean value and standard deviation of the 42-item PICASN can be seen in Table 2. However, upon excluding ten items (Q7, Q10, Q19, Q20, Q26, Q33, Q35, Q37, Q38, and Q39), the I-CVI and S-CVI improved to 0.94 and 0.88, respectively. The overall S-CVI reached an acceptable level of 0.88. Furthermore, based on an I-R correlation threshold of less than 0.6, five additional items (Q1, Q2, Q16, Q40, and Q42) were removed. Items with an I-R correlation of 0.6 or higher indicated high consistency and congruence between individual item measurements and the overall scale. Consequently, the final analysis retained 27 items with two extracted factors, which explained 80% of the variance.
| Item Number | Item Statement It is important for novice nurses to: | Mean | SD |
|---|---|---|---|
| Q1 | Greet patients positively | 4.44 | 0.73 |
| Q2 | Interact with patients intentionally | 4.46 | 0.68 |
| Q3 | Interact with patients with a caring attitude | 4.57 | 0.60 |
| Q4 | Develop a conversation tailored to the patient | 4.32 | 0.71 |
| Q5 | Ask questions to other nurses to ensure patient safety | 4.64 | 0.60 |
| Q6 | Speak from the patient’s point of view | 4.38 | 0.72 |
| Q7 | Have conversations with senior nurses based on the patient-centered care model | 4.22 | 0.79 |
| Q8 | Use an appropriate professional manner of language | 4.60 | 0.59 |
| Q9 | Dress and groom appropriately as expected of a nurse | 4.67 | 0.55 |
| Q10 | Act with humility toward others | 4.46 | 0.77 |
| Q11 | Make great efforts for self-study every day | 4.53 | 0.62 |
| Q12 | Talk intentionally with other staff nurses within the team | 4.40 | 0.66 |
| Q13 | Look up things they don’t understand on their own | 4.60 | 0.62 |
| Q14 | Ask questions after sorting out what they do not understand | 4.43 | 0.72 |
| Q15 | Understand senior nurses’ advice appropriately | 4.52 | 0.58 |
| Q16 | Talk to uncomfortable people | 3.64 | 1.19 |
| Q17 | Greet other staff in a positive manner | 4.56 | 0.65 |
| Q18 | Verbalize what I understand | 4.35 | 0.70 |
| Q19 | Use nonverbal expressions so that other people can feel that the nurses understood what I was saying | 4.16 | 0.81 |
| Q20 | Know what I can and cannot do | 4.56 | 0.61 |
| Q21 | Maintain an appropriate sense of distance from disagreeable nurses | 4.36 | 0.77 |
| Q22 | Be open to advice from other staff nurses | 4.44 | 0.70 |
| Q23 | Not become emotionally attached to the points raised by nurses in their team | 4.22 | 0.85 |
| Q24 | Be honest about my mistakes and not hide them | 4.67 | 0.57 |
| Q25 | Express their feelings to other staff nurses within their team during difficult times | 4.29 | 0.84 |
| Q26 | Self-disclose and make themselves understood in their team | 4.18 | 0.87 |
| Q27 | Proactively check with senior nurses when they are unsure about something in their work | 4.68 | 0.52 |
| Q28 | Report at the right time based on the senior nurses’ situation | 4.39 | 0.70 |
| Q29 | Adequately report their work progress to senior nurses | 4.52 | 0.58 |
| Q30 | Talk with senior nurses without hesitation | 4.23 | 0.85 |
| Q31 | Be specific about the nursing care they want to be supported by senior nurses | 4.41 | 0.67 |
| Q32 | Ask senior nurses to provide care, which I cannot do by myself | 4.51 | 0.66 |
| Q33 | Prioritize the senior nurses’ opinions over my own (* invert item) | 2.35 | 1.05 |
| Q34 | Actively listen to senior nurses’ past experiences for my own growth | 4.04 | 0.90 |
| Q35 | Identify senior nurses who have a negative influence in my department | 4.16 | 0.84 |
| Q36 | Find reliable seniors in my department | 4.50 | 0.64 |
| Q37 | Be concerned about the health of other nurses in their teams | 4.00 | 0.97 |
| Q38 | Have private conversations within the same team of nurses | 3.45 | 1.14 |
| Q39 | Identify people who have a negative influence on my growth | 4.15 | 0.81 |
| Q40 | Seek support from the nurses on their team so that they do not hold onto their concerns | 4.26 | 0.77 |
| Q41 | Convey words of gratitude to the senior nurses who taught them | 4.64 | 0.56 |
| Q42 | Proactively support busy nurses within their team | 4.24 | 0.83 |
Reliability Measure Results
The reliability measures for the two-factor structure of the PICASN (perception dimension, 27 items) demonstrated strong internal consistency. Specifically, the Basic Competencies as a Novice nurse (Factor 1), consisting of 15 items, had an excellent reliability of 0.94. Similarly, the Relationship Building Skills within the Healthcare Team (Factor 2), comprising 12 items, demonstrated a high internal consistency reliability of 0.91. The overall scale reliability was exceptionally high at 0.95, as indicated in Table 3.
| Extracted Factors | Factor Loadings | ||
|---|---|---|---|
| Factor 1 | Factor 2 | ||
| Item Number |
Factor 1: Basic Competencies as a Novice nurse (15 items) It is important for novice nurses to: |
||
| Q3 | Interact with patients with a caring attitude | 0.97 | |
| Q5 | Ask questions to other nurses to ensure patient safety | 0.94 | |
| Q8 | Use an appropriate professional manner of language | 0.89 | |
| Q9 | Dress and groom appropriately as expected of a nurse | 0.82 | |
| Q2 | Interact with patients intentionally | 0.77 | |
| Q4 | Develop a conversation tailored to the patient | 0.70 | |
| Q13 | Look up things they don’t understand on their own | 0.63 | |
| Q11 | Make great efforts for self-study every day | 0.59 | |
| Q15 | Understand senior nurses’ advice appropriately | 0.58 | |
| Q17 | Greet other staff in a positive manner | 0.57 | |
| Q14 | Ask questions after sorting out what they do not understand | 0.57 | |
| Q24 | Be honest about their mistakes and not hide them | 0.51 | |
| Q41 | Convey words of gratitude to the senior nurses who taught them | 0.49 | |
| Q6 | Speak from the patient’s point of view | 0.48 | |
| Q27 | Proactively check with senior nurses when they are unsure about something in their work | 0.48 | |
| Cronbach’s alpha = 0.94 | |||
|
Factor 2: Relationship-Building Skills within the Healthcare Team (12 items) It is important for novice nurses to: |
|||
| Q30 | Talk with senior nurses without hesitation | 0.83 | |
| Q31 | Be specific about the nursing care they want to be supported by senior nurses | 0.80 | |
| Q25 | Express their feelings to other staff nurses within their team during difficult times | 0.79 | |
| Q23 | Not become emotionally attached to the points raised by nurses in their team | 0.72 | |
| Q34 | Actively listen to senior nurses’ past experiences for their own growth | 0.71 | |
| Q32 | Ask senior nurses to provide care, which they cannot do by themselves | 0.67 | |
| Q22 | Be open to advice from other staff nurses | 0.63 | |
| Q29 | Adequately report their work progress to senior nurses | 0.63 | |
| Q18 | Verbalize what they understand | 0.61 | |
| Q36 | Find reliable seniors in their department | 0.55 | |
| Q42 | Proactively support busy nurses within their team | 0.49 | |
| Q28 | Report at the right time based on the senior nurses’ situation | 0.48 | |
| Cronbach’s alpha = 0.91 | |||
| Overall Cronbach’s alpha = 0.95 | |||
Discussion
The study sought to develop a reliable and valid tool for evaluating the interpersonal skills and competency required by novice nurses, taking into account Japanese cultural characteristics. The methodology in this study aligns with established literature standards, specifically employing EFA. The appropriateness of the dataset and sample sizes is affirmed by the KMO measure and Bartlett’s test of sphericity (Li & Lopez, 2007; Tabachnick & Fidell, 2007).
Through Promax rotation, two factors were extracted, explaining 80% of the variance. Promax rotation was chosen due to a factor correlation matrix yielding a correlation value of 0.712. DeVellis (2003) suggested that oblique rotation like Promax is preferable when factor correlations exceed 0.15. Out of the initially generated 42 items in the instrument development’s first step, 15 were eliminated based on content and construct validity. Ultimately, two factors were retained, comprising 27 items.
The first factor highlights essential competencies for novice nurses, emphasizing effective communication, continuous learning, professionalism, and accountability. Novice nurses are encouraged to approach their work compassionately, seek guidance, and actively engage in self-improvement. Acknowledging mistakes and expressing gratitude contribute to a positive work environment. Patient-centric care, consultation with experienced colleagues, and addressing patients’ families’ needs are crucial elements in ensuring quality nursing care, aligning with the theory of interpersonal relationships in nursing by Peplau (1997).
In pursuing patient-centered care, organizational behavior becomes crucial, consisting of understanding patients, caring for them, and building relationships (Bokhour et al., 2018). Nurses are responsible for nurturing trusting relationships with patients and their families, as the delivery of quality care relies on strong interpersonal skills and consideration for others (Jones, 2015). Recognizing the significance of attending to the needs of patients’ families is essential; however, reports indicate that establishing positive relationships with families can be challenging for some nurses (Holden et al., 2002).
Soft skills acquired by novice nurses play a pivotal role in enhancing the perceived satisfaction of patients and their families regarding the care received. Additionally, these soft skills contribute significantly to the overall quality of care and protect against mental health disorders, such as work-related stress or burnout (Sancho-Cantus et al., 2023). Furthermore, the soft skills required by novice nurses encompass the development of new communication skills, adaptability, and problem-solving abilities to assimilate advanced digital skills and digital knowledge (Isidori et al., 2022). It is worth noting that a majority of nurses express feeling underprepared in the soft skills of communication, professionalism, and leadership (Liebrecht & Montenery, 2016).
The second factor emphasizes cultivating relationship-building skills within the healthcare team. Effective communication and collaboration are pivotal for novice nurses. Open conversations with senior nurses facilitate knowledge exchange while maintaining emotional detachment and fostering a healthy work dynamic. Active listening to senior nurses’ experiences significantly contributes to professional development, and seeking assistance, providing progress reports, and identifying reliable mentors are essential components of a supportive work environment.
To continue growing professionally, novice nurses must build strong relationships with colleagues (James et al., 2021). Effective communication within the healthcare team is crucial for safety (Rodziewicz et al., 2018), and understanding unspoken cues is particularly significant in the Japanese context (Matsudaira et al., 2008). Collaborating with colleagues enhances self-awareness and knowledge and is vital during sudden patient changes and evolving treatments (James et al., 2021).
Nurses may feel distressed when dealing with medical errors, highlighting the need for a positive support system (Mok et al., 2020). As advocated by Tomooka et al. (2021), supportive interactions with the healthcare team create a culture where novice nurses are comfortable reporting errors and addressing concerns about patient safety.
The process of professional socialization for new graduate nurses, as outlined by Feng and Tsai (2012), involves adapting to the bureaucratic system and ward culture, highlighting the importance of understanding their transition experiences (Hussein et al., 2017). Navigating challenges and engaging in collaborative problem-solving contribute to the professional growth of novice nurses, making the nursing profession more rewarding and instilling pride in their work.
Implications for Nursing Education and Practice
The PICASN, designed for assessing and enhancing the interpersonal skills of novice nurses, plays a pivotal role in nursing education and practice. In educational settings, PICASN allows for establishing baseline assessments, enabling instructors to evaluate students’ initial competency levels and monitor progress over time. This dynamic feedback loop facilitates curriculum adjustments, ensuring that teaching strategies align with the evolving needs of novice nurses. The tool empowers novice nurses by fostering self-awareness and offering targeted insights into areas requiring improvement. In practice, PICASN provides experienced nurses and nurse managers valuable insights into team dynamics, guiding interventions for continuous quality improvement. The tool serves as a common language for discussing and addressing interpersonal skills, fostering enhanced communication and collaboration among healthcare teams. Ultimately, PICASN contributes to a positive work environment, aligning with best practices in nursing education and supporting the delivery of high-quality, patient-centered care.
Limitations of the Study and Recommendations
The study focused on developing and validating the PICASN within the Japanese cultural context, potentially limiting its generalizability to diverse cultural settings. Future research should investigate the cross-cultural applicability of the tool to ensure its relevance and effectiveness in assessing the interpersonal skills and competencies of novice nurses across various healthcare environments. Increasing the number of subjects through additional surveys and conducting confirmatory factor analysis will be necessary. The incongruence between perception and behavior should also be clarified. Conducting longitudinal studies to assess the predictive validity of the PICASN would offer valuable insights into its effectiveness in tracking the development of novice nurses’ interpersonal skills over time. Long-term observations can contribute to refining the tool and providing evidence of its utility in educational and practice settings.
Conclusion
The 27-item PICASN demonstrates adequate psychometric properties, with a high item and scale-content validity index and excellent internal consistency reliability. The PICASN is valuable for measuring professional interpersonal competency among novice nurses in Japan. In nursing education, the PICASN can be used for assessing and enhancing students’ interpersonal skills, enabling programs to monitor progress and customize learning experiences. In nursing practice, PICASN assists novice nurses in developing self-awareness and improving specific skills while providing experienced nurses and managers with insights into staff perceptions.