Heart failure (HF) is a complex clinical syndrome with a potential increase in prevalence and incidence annually. It disturbs physical and psychological health together with the quality of life (QOL) in both persons with HF and their families. The standard guidelines purpose to control HF symptoms, delay the progression of the disease, and improve self-care and the QOL using both guideline-directed medication therapy (GDMT) and various lifestyle modification, especially to constantly do a physical activity (PA) (Ponikowski et al., 2016).
PA is one of the essential self-care and is a class IA recommendation as it can decrease the exacerbation of HF symptoms, enhance the ability to accomplish daily activities, and promote QOL (Zores et al., 2019). Regarding the mechanisms of PA in persons with HF, PA can improve ventricular diastolic function by post-translational modification of protein titin, a critical protein cause of HF. Moreover, PA can increase the restoration of a healthy neurohormonal balance, increase respiratory muscle strength, enhance distensibility of pulmonary circulation (Nayor & Vasan, 2015). In Thailand, PA has been studied and well documented in healthy adolescents, adults, and older populations (Liangruenrom et al., 2019). However, lack of evidence to study PA in persons with cardiovascular disease, particularly in persons with HF.
PA is defined as the movement of the body by skeletal muscles as a result of energy expenditure, including household activities, occupational-related PA, recreational activities, sports, and transportations (Caspersen et al., 1985). There are several methods to measure PA, both direct and indirect methods. The direct methods including by accelerometers, pedometers, and fitness trackers, while the indirect methods include using a questionnaire and direct observation (Dowd et al., 2018). Furthermore, PA has been associated with many factors, even in healthy populations and persons with HF. The systematic reviews conducted abroad and in Thailand concluded that the variables, including personal factors, psychological factors, and environmental factors, were associated with PA. However, in Thailand, there is a lack of evidence to measure PA and its related factors in persons with HF, particularly the health status and health care system factors (Liangruenrom et al., 2019).
Nurses play an important role in promoting and increasing the level of PA in healthy populations across the lifespan and persons with complex chronic conditions. Nurses frequently contact, assess, recommend, and help motivate them to keep physically active (Vishnubala et al., 2020). Even though there is moderate evidence in promoting PA in persons with HF delivered by physiotherapists. However, lack of study focusing on promoting PA in persons with HF delivered by nurses (Amirova et al., 2021). Consequently, to study the relationship between PA and its related factors in persons with HF is necessary for nurses and health care providers (HCPs) to gain more understanding of PA and many factors, resulting in planning and providing appropriate interventions and recommendations in persons with HF.
Interestingly, the factors related to PA are based on the self-and family management framework, which is usually defined as the ability of individuals to incorporate with families, communities, and health care professionals. The framework is a dynamic, interactive, and daily process that individuals and families manage their chronic conditions (Grey et al., 2015). Factors based on the framework include motivation, functional ability, family support, and perceived quality of patient-provider relationships. The motivation was selected in this study to represent the personal factor since it is an essential factor associated with PA in persons with HF, especially in the initiation and maintenance of PA (Ha et al., 2018). Functional ability was selected to reflect the health status of persons with HF. Functional ability is described as the ability of a person to accomplish daily self-care activities. The persons with a higher ability to do activities in daily living potentially stay physically active in the long term (Tharp et al., 2019). In persons with HF, family resource factors, particularly better family support, have been linked to better self-care adherence and maintenance of PA (Dunbar et al., 2008; Shahriari et al., 2016). Additionally, a good relationship between patients and HCPs is highly related to maintaining PA in persons with HF (Currie et al., 2015; Tongtiam et al., 2016).
Consequently, the study aimed to determine the PA level among persons with HF and explore the relationship between PA and its related factors based on self-and family management framework in various dimensions, including motivation, functional ability, family support, and perceived quality of patient-provider relationships. The findings may help the persons with HF and HCPs understand the PA level and promote suitable recommendations for persons with HF.
Methods
Study Design
This research was a correlational cross-sectional study aimed to determine the PA level among persons with HF and explore the relationship between PA and its related factors based on self-and family management framework, including motivation, functional ability, family support, and perceived quality of patient-provider relationships.
Sample and Setting
The Multidisciplinary Heart Failure Clinic, an outpatient department of Faculty of Medicine Ramathibodi Hospital, Mahidol University, Bangkok, Thailand, was selected as the research setting. The clinic has been managing persons with HF using the multidisciplinary approach. These persons with HF received the diary and HF booklet and information needed for self-care, including adherence to medication recommendations, PA and appropriate exercise, consumption of a low-salt diet, restriction of fluid intake, cessation of tobacco and alcohol use, daily monitoring of body weight, and signs and symptoms of worsening HF from nurses and other HCPs. These participants were selected and included in the study using purposive sampling from December 2020 to May 2021. Inclusion criteria were 1) 18 years of age and older of persons with HF; 2) functionally classified as NYHA class I to III; 3) literate and able to speak and understand the Thai language; 4) willing to participate in this study, and 5) living with a family member. Exclusion criteria were 1) participants who have an activity limitation and immobilization; and 2) participants who have an acute and critical illness during participation in this study.
To compute the required sample size by the G-power, given α as .05, 80% of the power. The effect size from related studies ranged from .30 to .80 (Duncan et al., 2010; Tongtiam et al., 2016; Okunrintemi et al., 2017). A one-tailed hypothesis was considered because the relationship between PA and its related factors showed the same direction in literature reviews from abroad and in Thailand. Moreover, the number of study samples who received multidisciplinary care in Thailand was limited, and multicenter settings might affect the relationship between PA and the perceived quality of patient-provider relationships. Consequently, the researchers considerately set a one-tailed hypothesis for this study. Thus, the sample size may range from nine to at least 67 participants. Finally, the sample size of the study was 70 participants, which was considered adequate.
Instruments
The research instruments in this study were divided into two categories. The first category was the screening instruments which was the Thai version of Mini-Cog for screening the cognitive impairment in persons aged 60 years old and older. It is a short, concise, and valid cognitive screening test, and it was shown good interrater reliability (K = .80, p <.001, 95% CI .50–1.00) (Trongsakul et al., 2015). For this study, 34 potential participants had been assessed by the Mini-Cog. However, only 29 participants had passed the test, and five participants were excluded.
The second category was the data collection instruments, including:
The patient data record form comprises the demographic and health information developed by researchers was used to collect demographic and health information of persons with HF.
The Self-report Physical Activity Questionnaire (SPAQ-Thai version) to assess the level of PA. The SPAQ showed a good predictive validity and correlation with the six-minute walk test (r = .75, p < .05), a good concurrent validity with Actigraphy (r = .31, p < .01), test-retest reliability was .93, and the content validity index was .89. The total hours of PA were calculated into MET-Hr/week to divide PA into three levels of intensity; low PA (<10 MET-Hr/week); moderate PA (10-49 MET-Hr/week); and high PA (≥50 MET-Hr/week) (Visuthipanich et al., 2009).
The Exercise Motivation Index (EMI-Thai version) was an adapted questionnaire from 23 items to 15 related items for assessing exercise motivation in persons with HF by Klompstra (2016). The Cronbach’s alpha was .89-.92, with possible scores of the instrument ranging from 0 to 60, and with higher scores meaning higher motivation in PA (Klompstra, 2016).
The Modified Barthel Activities of Daily Index (MBAI-Thai version) was developed for assessing functional ability in older people with the Kappa coefficients of inter-rater reliability, and repeatability tests were .79 and .68, respectively (Jitapunkul et al., 1994).
The Social Support and Exercise Survey (SSE-Thai version) was developed to assess perceived family support to exercise behaviors. The test-retest reliability estimates for the family was .77, and Cronbach’s alpha was .91, possible scores of the instrument ranging from 12 to 60, with higher scores meaning higher perception of family support in PA (Kaewthummanukul et al., 2006).
The Modified Patient Reactions Assessment (MPRA-Thai version) was an instrument to assess the perception of the quality of patient-provider relationships. The coefficient alpha of the Thai version was .79, with possible total scores ranging from 15 to 105, and a higher overall score reflecting the greater relationship between persons and HCPs (Siripitayakunkit et al., 2008).
All instruments were permitted by the original authors and assessed to ensure face validity, content validity, and reliability by two nursing instructors and an advanced nurse practitioner with a Content Validity Index equal to 1. Only the EMI was translated from English into Thai version by two bilingual experts in Thai and English compared with the original version in conceptual, content, and construct equivalences across the two languages and cultures. The EMI has been tested its reliability in persons with HF who received multidisciplinary management and were already discharged from the HF clinic. The results showed that the Cronbach’s alpha of EMI was .883. In this study, the Cronbach’s alpha of the EMI, the SSE, and the MPRA were .918, .921, and .827, respectively. Thus, reflecting it is acceptable in the reliability of these research instruments.
Data Collection
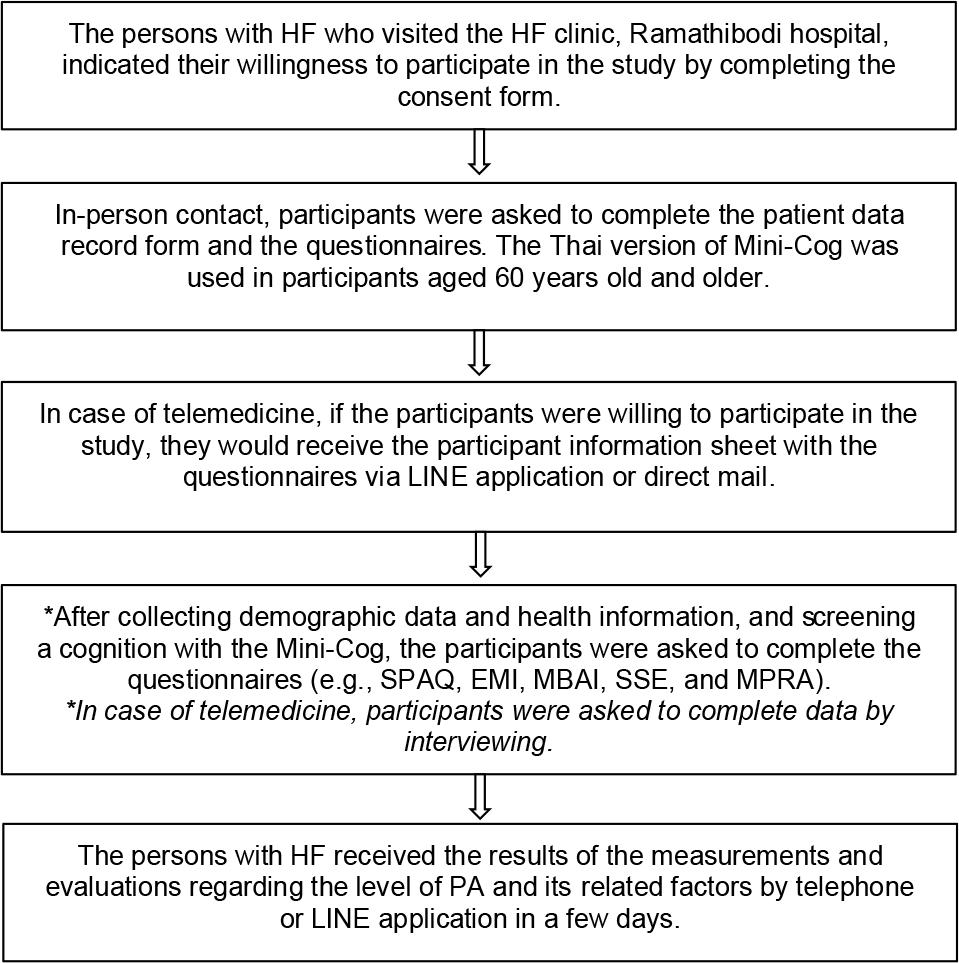
The data collection can be seen in Figure 1.
Data Analysis
The demographic data, health information, and the scores of the study variables were analyzed by use of descriptive statistics, including frequency, percentage, mean, range, and standard deviation. The PA data were analyzed using descriptive statistics and were calculated to identify MET-Hr/week. In the end, three levels of PA were classified: low, moderate, and high PA. The factors related to PA in persons with HF were analyzed using correlation coefficient statistics, and the magnitude of the correlation coefficient was stratified and applied from the related study (Schober et al., 2018).
The Pearson’s correlation coefficient was used, and it requires the following assumptions; firstly, the study variables were continuous variables. Secondly, all variables have a linear relationship with each other. Lastly, all variables have a bivariate normal distribution. The researchers have to use Spearman’s rank correlation coefficient if the data does not meet the above assumptions (Schober et al., 2018).
Ethical Consideration
The research was submitted to and approved by the Institutional Review Board, Faculty of Medicine Ramathibodi Hospital, Mahidol University, Thailand, with the approval number COA. MURA2020/1705. The potential participants were identified for the study and voluntarily consented to participate in this study. All of the data were kept confidential and anonymous using identification numbers. The confidentiality and freedom to withdraw from the study at any time were assured, and the participants were assured that their decisions would not affect the treatment and care.
Results
Participants’ Socio-Demographic Characteristics
A total of 82 potential participants were recruited from the Heart Failure Clinic, five participants might have a cognitive impairment, and seven participants could not be reached out. Therefore, 70 participants participated in the study. Regarding the socio-demographic data, most participants were male (70.00%), the mean age of participants was 54.21 (SD = 15.89) years. More than half of the participants (68.60%) were married, and all participants lived with their family members. When considering PA and exercise, most participants (84.30%) had space to do activities and exercises, and 40.00% had their exercise buddy (Table 1).
| Characteristics | Frequency | Percentage | |
|---|---|---|---|
| Gender | Male | 49 | 70.00 |
| Female | 21 | 30.00 | |
| Age (years) | Mean = 54.21 SD = 15.89 Range 19-83 years | ||
| Marital status | Single | 19 | 27.10 |
| Married | 48 | 68.60 | |
| Divorced/Separated | 1 | 1.40 | |
| Widowed | 2 | 2.90 | |
| Living with family members | Spouse/Partner | 36 | 51.40 |
| Son-Daughter | 14 | 20.00 | |
| Father-Mother | 13 | 18.60 | |
| Other relatives | 7 | 10.00 | |
| Area for exercise (at home) | Yes | 59 | 84.30 |
| No | 11 | 15.70 | |
| Exercise equipment (at home) | Yes | 33 | 47.10 |
| No | 37 | 52.90 | |
| Exercise place (in village/community) | Yes | 57 | 81.40 |
| No | 13 | 18.60 | |
| Exercise buddy | Yes | 28 | 40.00 |
| No | 42 | 60.00 | |
Clinical Characteristics of the Participants
A total of 70 participants were diagnosed with HF range from 1 to 65 months (Mean = 18.01, SD = 14.92). The majority of the participants were recently classified as NYHA class II, and they had comorbidities with hypertension, dyslipidemia, and diabetes mellitus. Ischemic heart disease and cardiac arrhythmia were facilitating factors inducing the progression of HF. More than half of the participants (55.70%) had heart failure with reduced ejection fraction (LVEF <40%). In addition, 81.40% had no cardiac device, 42.90% met the GDMT, and 61.40% had no hospitalization history (Table 2).
| Characteristics | Frequency | Percentage | |
|---|---|---|---|
| Time of diagnosis HF (months) | Range 1-65 months, Mean = 18.01, SD = 14.92 | ||
| NYHA classification | Class I | 21 | 30.00 |
| Class II | 47 | 67.10 | |
| Class III | 2 | 2.90 | |
| Comorbidity | Hypertension | 31 | 44.30 |
| Diabetes Mellitus | 21 | 30.00 | |
| Dyslipidemia | 22 | 31.40 | |
| Facilitating factor-induced HF | Ischemic heart disease | 32 | 45.70 |
| Cardiac arrhythmia | 24 | 34.30 | |
| Valvular heart disease | 8 | 11.40 | |
| The latest LVEF (%) | Range 18-82%, Mean = 39.55, SD = 16.21 | ||
| LVEF < 40% | 39 | 55.70 | |
| LVEF 40-49% | 11 | 15.70 | |
| LVEF ≥ 50% | 20 | 28.60 | |
| Cardiac device | Yes | 13 | 18.60 |
| No | 57 | 81.40 | |
| Meet guideline-directed medication therapy | Yes | 30 | 42.90 |
| No | 40 | 57.10 | |
| Previous admission within a year | No admission | 43 | 61.40 |
| Admission with a cardiac cause | 15 | 21.40 | |
| Admission with non-cardiac cause | 12 | 17.10 |
Note: HF = Heart failure, NYHA = New York heart association, LVEF = Left ventricular ejection fraction
Physical Activity of the Participants
The PA level of the participants (N = 70) was calculated into total metabolism hour per week (MET-Hr/week), 78.50% had a high PA level, and 21.50% had a moderate PA level. In addition, all participants met the PA recommendation. Regarding the average subscale of PA, most participants had high activity in recreational PA, followed by household PA and exercise (Table 3).
| Parameters | Min-Max | Frequency | Percentage |
|---|---|---|---|
| Level of PA (MET-Hr/week) | |||
| Low PA (<10 MET-Hr/Wk) | 0 | 0 | .00 |
| Moderate PA (10-49 MET-Hr/Wk) | 21.13-46.40 | 15 | 21.50 |
| High PA (≥ 50 MET-Hr/Wk) | 50.78-309.85 | 55 | 78.50 |
| Recommendations1 of PA (150 minutes/week) | |||
| Achieve (PA ≥ 150 minutes/week) | 600-6840 | 70 | 100.00 |
| Not Achieve (PA < 150 minutes/week) | 0 | 0 | .00 |
| Parameters | Min-Max | Mean | SD |
| Total PA (all items) | 21.13-309.85 | 82.37 | 49.93 |
| MET-Hr/Wk of household PA (item 1-13 of SPAQ) | 0-136.90 | 24.24 | 24.93 |
| MET-Hr/Wk of occupational PA (item 14-16 of SPAQ) | 0-40.00 | 4.58 | 8.35 |
| MET-Hr/Wk of recreational PA (item 17-27 of SPAQ) | 0-48.50 | 24.53 | 10.56 |
| MET-Hr/Wk of exercise PA (item 28-50 of SPAQ) | 0-155.00 | 18.85 | 24.27 |
| MET-Hr/Wk of transportation PA (item 51-54 of SPAQ) | 0-72.00 | 10.15 | 13.48 |
The Score of the Study Variables
The participants had a high overall motivation to be physically active. In addition, all participants had a high ability to do daily activities, most participants (70.00%) had independence, and the others (30.00%) had mild dependence. Furthermore, in family support, participants had a moderate perception of family support. Moreover, the results showed a high level of relationship between persons and providers (Table 4).
| Study variables | Possible range | Actual range | Mean (SD) |
|---|---|---|---|
| Motivation | 0-60 | 31-60 | 50.20 (7.26) |
| Physical motivation | 0-16 | 10-16 | 14.12 (1.80) |
| Psychological motivation | 0-16 | 9-16 | 14.04 (2.01) |
| Social motivation | 0-28 | 11-28 | 22.02 (4.27) |
| Functional ability | 0-20 | 15-20 | 19.44 (1.07) |
| Independence | 20 | 20 | 20.00 (.00) |
| mild dependence | 12-19 | 15-19 | 18.14 (1.19) |
| Family support | 12-60 | 13-60 | 30.77 (9.73) |
| Perceived quality of patient-provider relationships | 15-105 | 81-105 | 99.30 (4.69) |
The Correlation Between Physical Activity and Its Related Factors
All study variables, including the PA, motivation, family support, and perceived quality of patient-provider relationships, were examined and passed the general statistical assumptions of Pearson’s correlation coefficient. Functional ability was examined but not passed the general assumptions; therefore, the functional ability was used Spearman rank-order correlation coefficient. The parametric statistic can provide trustworthy results, and the non-parametric statistic was valid when our number of the study sample had a limitation. However, the number of study samples was limited. Therefore, to be especially careful in conclusion and generalizability.
The findings showed that a total PA had a significant positive correlation with a functional ability (rs = .309, p < .05), and family support (r = .210, p < .05). While the results showed PA had a non-significant positive correlation with motivation (r = .050, p > .05), and a non-significant negative correlation with perceived quality of patient-provider relationships (r = -.049, p > .05). The magnitude of the correlation coefficient was stratified and applied from the related study (Schober et al., 2018) (Table 5).
| Study variables | Physical activity |
|---|---|
| Motivation | r = .050 |
| Functional ability | rs = .309* |
| Family support | r = .210* |
| Patient-provider relationships | r = -.049 |
Note: r = Pearson’s Correlation Coefficient; rs = Spearman’s Rank Correlation Coefficient,
Discussion
The research findings showed that a majority of participants had a moderate and high level of PA, and all participants met the PA recommendation. These findings were consistent with the related study, which reported that the majority of persons with HF had a moderate and high PA (Klompstra, 2016). To support the study findings, it was found that most participants in the study were men, the average age of the participants was 54 years old, and they were classified in NYHA classes I and II. Furthermore, approximately half of the participants have met the GDMT, and the majority of participants had no cardiac devices and a hospitalization history in the previous year. Consequently, most participants may have had more chances to do PA without adverse events. However, it would be better to assess PA in subjective and objective ways to ensure that the researchers receive reliable and accurate information regarding PA (Dowd et al., 2018).
In this study, the findings revealed that PA had a non-significant positive correlation with motivation (r = .050, p > .05). It was not congruent with the result from a previous study that reported motivation had a significant positive correlation with PA (Klompstra, 2016). The study findings found that most participants had high motivation in all aspects. Although their motivation scores in keeping physically active were high, motivation may have less variation across the participants. Therefore, it might affect the correlation between PA and motivation in real life.
The research findings showed that functional ability had a significant positive correlation with PA (rs = .309, p < .05). It was not surprising to find that functional ability had a correlation with PA for the reason that functional ability plays an important role in HF. When the persons have a low ability to perform their daily activities, their PA might potentially decrease (Tongtiam et al., 2016). These findings demonstrated that using functional ability may reflect the health status of persons with HF. However, using the functional ability may inherently overlap with PA and result in a significant positive correlation between functional ability and PA. To enhance the PA, HCPs have to consider the confounding factors such as age and gender differences which might influence PA level before offering suggestions and recommendations PA for the persons with HF (Amirova et al., 2021).
This study also showed that family support had a significant positive correlation with PA in persons with HF (r = .210, p < .05). It is shown that a majority of participants were married, lived with their family members, and almost half of the participants exercised and performed activities with their family members. The results were congruent with other studies that demonstrated that family support had a statistically significant relationship with self-care behaviors, including regular exercise and PA (Liangruenrom et al., 2019). Therefore, HCPs should integrate the participation of family supports to provide appropriate interventions for persons with HF.
Surprisingly, the PA had a non-significant correlation with perceived quality patient-provider relationships (r = -.049, p > .05). The possible reasons to explain the result, whether the participants in the HF clinic had a low, moderate, or high level of PA, they were usually satisfied with and had a good relationship with HCPs. When considering the method to assess the relationship, it could be explained that negative and positive items in the questionnaires might have influenced the rating scores of the participants (Solis Salazar, 2015). Moreover, the questionnaire was a generic instrument to assess the clients’ satisfaction and patient-provider relationships; however, it was not a specific questionnaire to assess the perceived quality of patient-provider relationships and PA in persons with HF.
In conclusion, the self-and family management framework was useful in providing guidelines for this study. The framework is defined as the ability of a person, family, community, and health care professional to manage chronic conditions (Ryan & Sawin, 2009; Grey et al., 2015). The study findings supported the assumptions, which consisted of a dynamic, interactive, and daily process to manage their conditions. Engaging the PA in persons with HF was influenced not only by the health status factors but also by the family resource factors, particularly the functional ability and family support in keeping physically active. Although motivation and perceived quality of patient-provider relationships were not related to PA in this study; however, these factors might enhance persons with HF to engage with PA and continuation of care (Chipidza et al., 2015).
The implication of this study for nursing practice, the findings of the study supported the fact that there were functional ability and family support related to the PA in persons with HF. Even though the motivation and perceived quality of patient-provider relationships were not associated with PA, these were essential factors to promote the patient’s self-care, especially in encouraging and maintaining the level of PA in persons with HF (Lobelo & de Quevedo, 2016). Currently, Thailand and various countries around the world are experiencing the rapid growth of the aging population and technology advancements affecting the increase of sedentary lifestyles. Therefore, these are the challenging issues that nurses have to manage and decrease their sedentary lifestyles. Moreover, it is necessary to provide the strategy in enhancing and maintaining PA in long-term care at both national and global levels.
A limitation of this study was that the study design was a cross-sectional study. The participants may have a lower or higher PA level, and the PA may be affected and changed at any time, especially in the COVID-19 situations. Purposive sampling was used in this study, resulting in a selection bias of the study sample. Additionally, the research setting as a single-center, multidisciplinary approach and the university-affiliated hospital might influence and increase the PA level in persons with HF. At best, the results of this study are generalizable to persons with HF at a similar level to the research setting.
Conclusion
The findings from this study demonstrated that persons with HF had suitable PA levels and met the PA recommendations. The functional ability and family support play an accountable role in keeping and maintaining PA. However, motivation and perceived quality of patient-provider relationships need to be further investigated. Based on the results of this study, we recommend that HCPs have to recognize these essential factors related to PA, especially to cooperate with the participation of the patient, family, community, and health care system for providing more effectively appropriate recommendations and suggestions among persons with HF in long-term care.